International Journal of Radiology and Radiation Oncology
A case of extremity over-exposure and regulatory compliance
1Department of Internal Medicine, Marshall University, Joan C. Edwards School of Medicine, Mountain Health Network, 1340 Hal Greer Blvd., Huntington, WV 25701, USA
2Department of Radiation Safety, Medical Affairs, 1340 Hal Greer Blvd., Huntington, WV 25701, USA
3Department of Radiology, Cabell Huntington Hospital, 1340 Hal Greer Blvd., Huntington, WV 25701, USA
4Medical Physicist, Radiology, Inc., 5221 US 60 East, Huntington, WV 25701, USA
Author and article information
Cite this as
Burdick HJ, Shoemaker T, Godby N, Norweck J (2023) A case of extremity over-exposure and regulatory compliance. Int J Radiol Radiat Oncol. 2023; 9(1): 5-7. Available from: 10.17352/ijrro.000050
Copyright License
© 2023 Burdick HJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.During a routine NRC inspection, a review of historical occupational dosimetry monitoring data for interventional radiology physician AUs was questioned regarding unexpectedly low results. This was interpreted to be an indicator of noncompliance with the wearing of occupational dose monitoring devices and, therefore, required occupation dose reconstructions in order to estimate the actual dose. In an effort to comply with dose monitoring requirements, the AU interventional radiologists diligently began wearing their whole-body and ring dosimeters during all procedures including Y-90, fluoroscopy-guided and CT-guided. In the interest of patient care, an AU that performs many interventional CT-guided procedures involving the use of a cumbersome treatment device, placed his hand in the CT beam on numerous occasions to stabilize the device. This quickly resulted in a cumulative extremity exposure that exceeded allowed limits. Once we became aware of the extremity over-exposure, steps were taken to prevent any further significant extremity exposure for the remainder of the year. The over-exposure was reported to the NRC and State following regulatory requirements.
Reconstruction of whole-body and extremity dose from x-ray and radioactive materials was completed on all interventional radiologists listed as Authorized Users (AU) of byproduct material under 10. CFR 35.1000 on our license. The radiation safety officer in collaboration with the NRC physicist created an experimental setup to measure the scattered dose per patient dose indicator. A digital ion chamber was used to measure the accumulated exposure at the usual physician position. An mR per mGy of indicated air kerma (AK) conversion factor was determined for fluoroscopy and mR per CTDIvol (mGy) for CT-guided procedures [1-5]. Dose reduction correction factors were applied to account for the use of protective lead equipment such as leaded gloves, eyewear, and ceiling-mounted shields. The completed dose reconstructions indicated several AUs listed on the license exceeded annual occupational dose limits during 2019 and 2021 (ML22073A220) [6-10].
Discussion
Due to gaps related to training and oversight of the radiation protection program, our facility has devoted a new full-time radiation safety assistant staff position, increased administrative oversite and training modules, and is routinely assessing and improving our radiation protection program. Rounding observations in areas that use radiation-generating devices and radioactive materials, increasing a positive radiation safety culture that includes an event reporting tool for those who want to report an unsafe event or exposure. We have also added a “Radiation Safety Huddle” distributed to all staff members quarterly.
Most facilities, (including our own), set forth ALARA overexposure limits for periodical review and reporting. Once a user reaches that limit or above, a formal notification and investigation occur at our facility [11-15]. Although it is not regulatory guidance, auditing for lower-than-expected dosimeter readings may indicate non-compliance with personnel monitoring. We created a subcommittee comprised of a responsible contact person designated as a badge coordinator to help with employee participation and to assist in the investigation of both underexposure and overexposure. Recognition, investigation, training, and escalated enforcement of non-compliance are tools we anticipate to improve radiation personnel dosimetry compliance [16-20].
Corrective action and follow ups
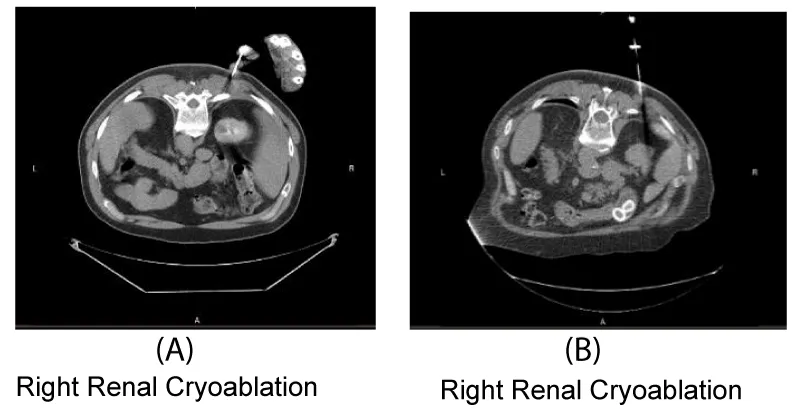
During the course of the over-exposure investigation and subsequent NRC and State reactive inspections, an extensive review of physician’s cases for the past three years revealed hand exposure in CT beam, in particular, CT-guided procedures (Figure 1A). The exceeded extremity overexposure was reviewed with the authorized user describing the possible radiation effects including a dermatological event. The overexposed physician reported no cutaneous radiation injury effects at this time. The AU expressed concern for overall safety and has improved the technique for CT-guided procedures where hand exposure is no longer seen in CT-guided cases after an extensive review for the last fourteen months (Figure 1B). Follow-up measures include a dermatologist consult where no radiation effects were noted.
Based on the given information, it was concluded that a workflow practice specific to positioning patients while the beam was on for biopsies and ablations was the root cause for the elevated extremity dose with very little exposure being due to the use of radioactive materials during Y-90 procedures. A review of the training records for the interventional radiology physician AUs also showed poor compliance with 10 CFR 19.12. 10 CFR 19.12 provides no exemption from training requirements for physicians based on their assumed knowledge from education, experience, and credentials. The assumption physicians were properly trained and knowledgeable as authorized users of by-product material or privileged fluoroscopy users, but as the responsible owner of the NRC license, the organization must verify radiation safety compliance.
We have implemented changes to improve the proper use of protective devices and encouraged physicians to use forceps or other medical equipment to eliminate hand in the beam, [2]. In addition to lead protective devices, shielding was put in place, (table skirt, Mavig Shields, sterile leaded gloves), and additional signage was posted on CT machines “Do not place hand in beam” and “Radiation dosimeters required beyond this point” before entering CT/Interventional Radiology suites to help reduce physician and staff exposures. There has been significant improvement and no hands in the beam have been seen in the audits of CT-guided procedures for the last 14 months. The radiation safety observations and CT-guided procedures audits are in place to eliminate reoccurrence.
After our initial NRC inspection, we became aware of NRC Information Notice 2021-02 which highlights similar issues associated with monitoring occupational exposure to radiation from licensed and unlicensed radiation sources. (ML21152A239). Based on our experience, it appears that this Information Notice is not widely distributed to those implementing the radiation protection program. We cannot overemphasize that this NRC Information Notice is of extreme importance, and it is critical for organizations to take it seriously.
Conclusion
The use of a ring radiation monitoring device for hand exposure to radioactive isotopes led to an unexpected finding of significant hand exposure from CT beams during CT- guided procedures and also led to successful corrective action plans in partnership with the U.S. Nuclear Regulatory Commission (NRC).
- Nuclear Regulatory Commission. (2021-06) NRC Inspection Report ML22073A220. NRC’s Agencywide Documents and Management System (ADAMS). https://www.nrc.gov/reading-rm/adams.html
- Sarmento S, Pereira JS, Sousa MJ, Cunha LT, Dias AG, Pereira MF, Oliveira AD, Cardoso JV, Santos LM, Santos JAM, Alves JG. The use of needle holders in CTF guided biopsies as a dose reduction tool. J Appl Clin Med Phys. 2018 Jan;19(1):250-258. doi: 10.1002/acm2.12234. Epub 2017 Nov 29. PMID: 29193644; PMCID: PMC5768016.
- International Atomic Energy Agency. Good practices in interventional procedures. https://www.iaea.org/resources/rpop/health-professionals/interventional-procuedures/good-practices-in-interventional-fluoroscopy
- Nuclear Regulatory Commission. (2021-02) NRC Information Notice ML21152A239. NRC’s Agencywide Documents and Management System (ADAMS) https://www.nrc.gov/reading-rm/adams.html
- Nuclear Regulatory Commission (U.S. NRC, n.d.) part 35—medical use of byproduct material | NRC.gov
- Nuclear Regulatory Commission (U.S. NRC, n.d.) Information For Radiation Workers | NRC.gov
- Bartal G, Vano E, Paulo G, Miller DL. Management of patient and staff radiation dose in interventional radiology: current concepts. Cardiovasc Intervent Radiol. 2014 Apr;37(2):289-98. doi: 10.1007/s00270-013-0685-0. Epub 2013 Jul 16. PMID: 23860936.
- Radiation Burn (Dermatitis): What it is, Treatment, Management. (n.d.). Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/21995-radiation-burns
- Fluoroscopy Safety and Radiation Exposure- ASRT Education. (n.d.). Www.asrt.org.
- Gerasia R, Ligresti D, Cipolletta F, Granata A, Tarantino I, Barresi L, Amata M, Benenati S, Gallo G, Tafaro C, Miraglia R, Traina M. Endoscopist's occupational dose evaluation related to correct wearing of dosimeter during X-ray-guided procedures. Endosc Int Open. 2019 Mar;7(3):E367-E371. doi: 10.1055/a-0841-3350. Epub 2019 Feb 28. Erratum in: Endosc Int Open. 2019 Mar;7(3):C1. PMID: 30834296; PMCID: PMC6395086.
- Nuclear Regulatory Commission (U.S. NRC, n.d.) Authorized Individuals | NRC.gov
- Furlow B. CT-Guided Interventional Radiology. Radiol Technol. 2019 Jul;90(6):581CT-597CT. PMID: 31270267.
- American Board of Radiology. Compliance with NRC Regulations. 2021. https://www.theabr.org/diagnostic-radiology/initial-certification/nrc-compliance
- Miller DL, Vanó E, Bartal G, Balter S, Dixon R, Padovani R, De Baère T. Occupational radiation protection in interventional radiology: a joint guideline of the Cardiovascular and Interventional Radiology Society of Europe and the Society of Interventional Radiology. Cardiovascular and Interventional Radiology. 2010; 33:230-239.
- Tonkopi E, Lightfoot C, LeBlanc E. SU‐F‐I‐72: Evaluation of the Ancillary Lead Shielding for Optimizing Radiation Protection in the Interventional Radiology Department. Medical Physics. 2016; 43(6Part8): 3403-3403.
- Re BJ. Yttrium-90 microsphere brachytherapy sources and devices TheraSphere® and SIR-Spheres®; comments of the American College of Radiology. American College of Radiology website.
- Seager M, Kumar S, Lim E, Munneke G, Bandula S, Walkden M. Renal cryoablation - a practical guide for interventional radiologists. Br J Radiol. 2021 Feb 1;94(1118):20200854. doi: 10.1259/bjr.20200854. Epub 2020 Sep 22. PMID: 32960674; PMCID: PMC7934314.
- Jaschke W, Schmuth M, Trianni A, Bartal G. Radiation-Induced Skin Injuries to Patients: What the Interventional Radiologist Needs to Know. Cardiovasc Intervent Radiol. 2017 Aug;40(8):1131-1140. doi: 10.1007/s00270-017-1674-5. Epub 2017 May 11. PMID: 28497187; PMCID: PMC5489635.
- Hricak H, Brenner DJ, Adelstein SJ, Frush DP, Hall EJ, Howell RW, McCollough CH, Mettler FA, Pearce MS, Suleiman OH, Thrall JH, Wagner LK. Managing radiation use in medical imaging: a multifaceted challenge. Radiology. 2011 Mar;258(3):889-905. doi: 10.1148/radiol.10101157. Epub 2010 Dec 16. PMID: 21163918.
- Wagner JB. Radiation Protection and Safety in Interventional Radiology. Radiol Technol. 2020 May;91(5):431-442. PMID: 32381661.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
