International Journal of Immunotherapy and Cancer Research
Probiotics and Bone Health: It takes GUTS to Improve Bone Density
1Osteoimmunology Lab, Department of Zoology, School of Biological Sciences, Dr. H S Gour Central University, Sagar (MP)-470003, India
2Institute of Bioinformatics & Biotechnology, Savitribai Phule Pune University, Pune-411007, India
Author and article information
Cite this as
Yousf H, Tomar GB, Kr Srivastava R (2015) Probiotics and Bone Health: It takes GUTS to Improve Bone Density. Int J Immunother Cancer Res. 2015; 1(1): 18-22. Available from: 10.17352/2455-8591.000005
Copyright License
© 2015 Yousf H et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Probiotics are a class of symbiotic bacteria whose administration in adequate amount provides health benefits to the host by altering the composition of gut microbiota. The gut microbiota is known to regulate both the host immune system and metabolism, leading to increased bone mass by inhibiting bone resorption. Ovariectomy induced estrogen deficiency which mimics postmenopausal osteoporosis in women leads to enhanced bone inflammation and resorption. Recently it has been reported that different strains of bacteria (e.g. Lactobacillus, Bifidobacteria etc.), have important role in gut-bone regulation in ovariectomized mouse. Thus administration of probiotics can open up new avenues in treatment of various inflammatory bone conditions such as osteoporosis and rheumatoid arthritis by modulating the delicate balance between the gut microbiota and immune system.
The commensal gut microbiota (GM) in our intestine performs various useful functions by modulating both the metabolism and immune status of the host [1]. The importance of the GM for both health and disease has been an active area of research in the recent past. The composition of GM is modulated by a number of environmental factors such as diet, antibiotic treatments or pathogens. Prebiotics on the other end are non-digestible food supplements that exert a health-promoting effect on the host by selectively stimulating the growth and activity of various bacteria residing within the gastrointestinal tract [2]. Probiotics literally means “for life” and the definition of probiotics has been varied since it was first coined [3]. Probiotics are mostly commensal bacteria residing in the gut. Probiotics are defined as live commensal microorganisms such as bacteria or fungi which when administered in adequate amounts can confer a health benefit on the host by altering the composition of the GM. Probiotics also positively affect the immune responses in the host gastrointestinal tract thereby promoting health. Some of the probiotics are bacterial components comprising of normal human intestinal flora which produce various beneficial end products such as short chain fatty acids and lactate metabolism. These bacterial populations have the potential to treat different clinical conditions [4], including osteoporosis, diabetes, fatty liver disease, inflammatory bowel disease (IBD) and cardiovascular disease (CVD) [5,6].
One of the key bone diseases associated with aging and postmenopausal condition is osteoporosis which affects more than 75 million people in Europe, Japan, and the USA. It is estimated that by the end of 2020 more than 60 million men and women will be suffering from osteoporosis [7]. Menopause is a major risk factor for osteoporosis. In fact fifty percent of the women population over the age of 50 will experience an osteoporosis-related fracture in their lifetime [8]. Also there is elevated risk of wrist, hip, or spine fracture due to osteoporosis which is estimated to be parallel to the risk of heart disease [9].The current review specifically focus on the vital role of probiotics in regulating bone health, which itself is modulated by the host immune system.
Gut microbiota and immune system
A cross talk between the host mucosal innate immunity and GM augments the growth, survival and homeostasis of the gut ecosystem. The GM plays a primary role in the induction, education, and function of the host immune system. On the other hand the immune system has principally evolved as a means to maintain the symbiotic relationship of the host with these highly diverse and evolving microbes. The resulting microbiota-immune system association allows the induction and maintenance of various regulatory pathways involved in tolerance to these diverse antigens [10]. A characteristic feature of the innate immunity is its ability to distinguish between beneficial and pathogenic microbes by the help of various “pattern recognition receptors” (PRRs). The toll-like receptors (TLRs) enable the cells to recognize highly conserved and diverse molecules on the surface of microorganisms, collectively called as pathogen-associated molecular patterns (PAMPs) [11]. Since these molecules e.g. lipopolysaccharides, peptidoglycans, flagellin and others, are also present on various commensal bacteria, they are often called as microbe-associated molecular patterns (MAMPs). The GM regulates the intestinal immunity by modulating the expression of TLRs on immune cells surface through MAMPs. The GM shapes the T cell repertoire in the lamina propria along with modulating the homeostasis of the host [12]. These mucosal T cells function as important mediators for not only the defense against intestinal pathogens, but they also help in wound healing, barrier repair and regeneration at sites of infection and injury [13]. T cells depending upon the environment milieu, which is regulated by the presence of various cytokines can either drive a pro-inflammatory (TH1, TH2 and TH17 cells) or an anti-inflammatory immune response (regulatory T cells-Tregs) [14]. Antibodies (mainly IgA) specific for intestinal bacteria is secreted with the help of intestinal dendritic cells (DCs) that sample the various bacteria penetrating the gut epithelium. These bacteria-laden DCs interact with B and T cells in the Peyer's patches and activate B cells to produce IgA specific against the intestinal bacteria [15]. Thus, IgA (a key player in barrier homeostasis) secreted by plasma B cells residing in the lamina propria, binds to the microbial antigens present in the gut lumen and prevent there translocation and infection [16]. The differentiation of B cells into IgA-producing plasma cells is induced via the stimulation of TLR5 on DCs by GM derived flagellin [17]. The intestinal microbiota is also responsible for modulating the development of invariant NK T cells (iNKT cells) responsible for various inflammatory immune responses [18]. Thus both the intestinal innate and adaptive immunity go hand in hand in maintaining homeostasis of the gut microenvironment [13].
Interplay between bone and immune system
The skeleton is continually being remodeled by the activity of bone-forming osteoblasts (OBs) and bone-resorbing osteoclasts (OCLs) [20]. OBs are derived from mesenchymal stromal cells whereas OCLs are derived from hematopoietic stem cells which are also the progenitors of immune cells [21]. OCLs are distinctively derived from myeloid-monocyte lineage of hematopoietic cells under the influence of local microenvironment. Macrophage colony stimulating factor (M-CSF) induces proliferation and up-regulated expression of receptor activator of nuclear factor-κB (RANK) on OCL precursor cells. This results in binding of RANK ligand (RANKL) on its receptor RANK present on the surface of OCL precursors leading to enhanced osteoclastogenesis [21]. Any imbalance between the processes of osteoclastogenesis and osteoblastogenesis results into the induction of various inflammatory bone diseases such as rheumatoid arthritis (RA) and osteoporosis [22]. The effect of inflammation on bone loss is well established. In various auto-immune diseases such as rheumatoid arthritis, osteoclastic bone resorption is driven mainly by the secretion of various inflammatory cytokines produced by T cells [23]. During menopause the resulting estrogen deficiency leads to enhanced formation and survival of OCLs. This effect is in part modulated due to loss of the immunosuppressive effects of estrogen, resulting in enhanced production of cytokines by T cells (Th17 cells) thereby promoting osteoclastogenesis [24].
Probiotics and bone health
Recent studies demonstrate that the GM regulates bone mass and this effect of the GM on bone mass is mediated mainly via its effect on the host immune system, which in turn regulates osteoclastogenesis. In one such study different strains of bacteria such as Lactobacillus and Bifidobacterium were shown to have the potential to escalate the bone mineral density in ovariectomized (ovx) rats and mice which simulate postmenopausal conditions of osteoporosis [25,26]. In another study the administration of Lactobacillus paracasei (NTU 101) and Lactobacillus plantarum (NTU 102) fermented milk to ovx mice resulted in higher trabecular number compared to ovx and sham-ovariectomized control groups [27]. Administration of Lactobacillus helveticus in male osteoporotic rats is reported to enhance both the bone mineral density and content (BMD and BMC) [28]. Similarly different studies with strains of Lactobacillus casei, Lactobacillus reuteri, and Lactobacillus gasseri described higher bone weight among the probiotic fed group with respect to control groups [29]. A recent study showed a significant reduction in bone resorption by L. reuteri via decreasing levels of tumor necrosis factor (TNF), thereby increasing BMD, BMC, trabecular number and thickness, along-with decreased trabecular space in both vertebral and femoral bones [25]. Strains of Bifidobacterium longum have also been studied to significantly affect bone health [29]. A reduced number of TRAP positive osteoclasts were found in groups fed with fermented broccoli compared to the control groups, while no significant differences were observed in body weight of rats between the groups [30]. Probiotics could also have a potential effect on bone build-up, which can be independent to that of prebiotics. This could occur via microbial synthesis of various metabolites and enzymes or synthesis of several vitamins [31] such as vitamin D, C, or K [32] or folate [33]. Based on these reports one may expect that the optimum combination or use of probiotics and prebiotics would deliver best results, which ultimately depends on the nature of disease or risk being considered. A comparative account of the various studies dealing with the effect of probiotics on bone health is charted in Table1 for ready reference.
The anti-inflammatory effects exerted by various probiotic bacteria are thought to be mediated via the induction of Treg cells [34]. Probiotic treatment has been found to reduce the expression of several osteolytic cytokines (TNFα and IL-1β), responsible for altered RANKL/ osteoprotegerin (OPG) ratio in cortical bone. These findings clearly signify that probiotic treatment alters the status of immune cells in the bone microenvironment resulting in attenuated bone resorption observed in ovx mice [35]. TNFα promotes osteoclastogenesis by stimulating expression of RANKL from bone marrow stromal cells and osteoblasts resulting in enhanced osteoclastogenesis from OCL precursor cells via RANKL [36]. OPG inhibits OCL differentiation in a dose dependant manner [37]. These findings clearly delineate the role of probiotic treatment in suppressing osteoclastogenesis. Administration of L. reuteri in mice alters the GM composition and prevents ovx-induced trabecular bone loss and resorption [8]. Also treatment of L. reuteri suppressed the percentage of CD4+ T cells in bone marrow, supporting the notion that GM has immunomodulatory properties and affects OCL-mediated bone resorption. In a separate study, oral administration of L. reuteri treatment was shown to decrease intestinal inflammation and increase trabecular bone mass in gonadal intact male mice [25]. This decrease in the number of CD4+ T cells in bone marrow in GF mice was a consequence of the impact of the GM on the adaptive immune system, leading to fewer CD4+ cells recirculating in the blood and secondary lymphoid tissue.
Rheumatoid arthritis (RA) is a systemic autoimmune disease characterized by inflammation of synovial joints with an increased expression of inflammatory cytokines [38]. TNFα is one of the critical cytokines in the pathogenesis of RA [39]. Patients with psoriatic arthritis and mice with TNFα-induced arthritis have increased numbers of circulating OCL precursors [40]. Treg cells are critical for maintaining self-tolerance and negatively regulate immune responses. Several strains of Lactobacillus have been reported to have therapeutic effect in experimental mouse models of inflammatory bowel disease, atopic dermatitis, and rheumatoid arthritis, and are associated with enrichment of Treg cells in the inflamed regions [41]. This inhibitory effect of probiotic L. strains was recently shown to depend on suppressive motifs in the DNA enriched in these strains that potently prevented dendritic cell activation and maintained Treg cell conversion during inflammation [42]. TGFβ is crucial for the activation, differentiation and activity of Treg cells [43]. Interestingly, in one study it was reported that ovx decreases the number of Treg cells in bone marrow in control but not probiotic treated mice. Furthermore, the expression of TGFβ1 was increased by probiotic treatment compared to control groups after ovx, suggesting the role of probiotics in Treg cell differentiation via induction of TGFβ1. In vitro studies have also shown that Treg cells directly inhibit OCL differentiation and function and this effect of Treg cells is stimulated by estrogen [44]. In addition, adoptive transfer of Treg cells decreases the number of OCLs and limits bone loss in ovx mice [45]. Collectively these findings suggest the immune-suppressive effect of probiotic treatment under various inflammatory conditions.
There could be a number of various possible mechanisms which could simultaneously exist for the effect of probiotics on bone. One of the potential effects of probiotics on bone could possibly occurs via the synthesis of vitamins [46].Vitamins like C, D, K, along with folate are involved in metabolism of calcium, a necessary component for bone formation [47]. Moreover, various strains of bacteria produce several short chain fatty acids which decrease parathyroid hormone thereby resulting in an increase in mineral absorption [48]. A recent study showed another mechanism in which intake of probiotics reduce intestinal inflammation and increased BMD, implying that GM have a significant effect on bone health [49]. The bacterial strain Lactobacillus reuteri 6475 have been reported to reduce pro inflammatory cytokine levels systemically, leading to increased bone volume fraction by reducing the expression of pro inflammatory cytokines in both Jejunum and ileum [25]. As several studies indicate that the GM modulates the magnitude of the bone loss in sex-steroid-deficient female mice, it was hypothesized that treatment with probiotics might protect mice from ovx-induced bone loss [50]. Different studies till date point that probiotic treatment reduces the expression of various inflammatory cytokines such as TNFα, IL-1β etc. and subsequently increased the expression of OPG, a potent inhibitor of osteoclastogenesis, in bone of ovx mice resulting in enhanced bone turnover. Currently very few and limited number of available probiotic strains have been explored for their effect on bone physiology, thus a detailed study is still awaited to uncap the huge potential inherent in this field of biology.
Future perspectives
In summary, it appears that the GM modulates both the host metabolism and immune status. Studies using germ free mice (GF) demonstrate that the GM is a regulator of bone mass and proposed that the inhibitory effect of the GM on bone mass is mediated via its effects on immune status, which also regulates osteoclastogenesis. A role of the GM in bone metabolism is further supported by various studies demonstrating that antibiotic, probiotic, and prebiotic treatments that impact GM composition regulate bone metabolism. Probiotics act by altering the composition or the metabolic activity of the GM [39]. The suggested underlying mechanisms for how probiotics contribute to health are manifold including increased solubility and absorption of minerals, enhanced barrier function and modulation of the immune system [51]. Probiotics are increasingly being used worldwide to treat various health issues. Studies indicate that probiotics may be effective in the treatment of some gastrointestinal diseases such as colic, irritable bowel, and inflammatory bowel disease [52]. In addition, probiotics have also showed promise in ameliorating other ailments that are distal to the gut, including eczema, asthma, and allergies [53].
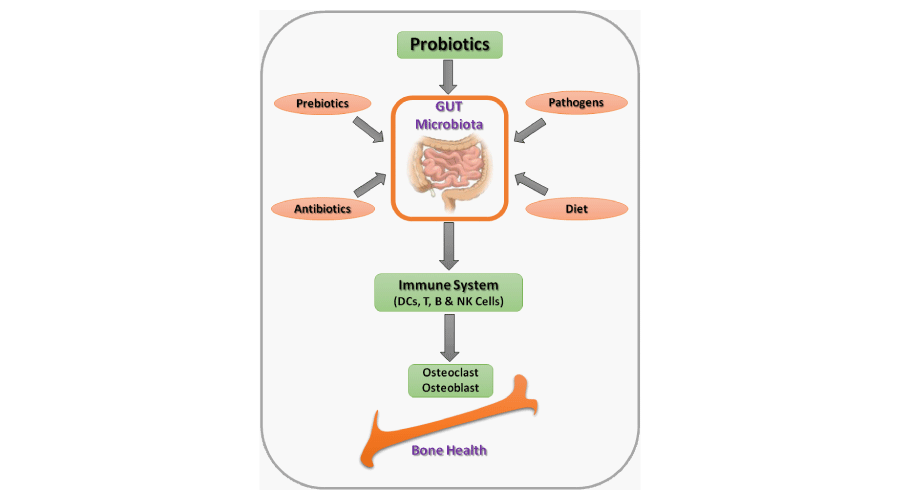
Current studies have shown that bone loss caused by sex-steroid deficiency is diminished in GF mice and can be prevented by treatment with various probiotics. Collectively, these studies suggest that GM may be a novel therapeutic target in osteoporosis (Figure 1). Treatment with probiotics has already been shown to improve bone mass in rodent models of bone loss. Thus future randomized clinical trials are required to determine the possible effect of probiotics along with various other novel therapies which have the potential to modulate the GM composition. Thus the role of GM in regulating the host immune system which in turn regulate bone mass validates the use of probiotics as possible novel therapeutics in treatment of various inflammatory bone conditions such as osteoporosis and RA.
Acknowledgement
This work was financially supported by a project from UGC Faculty Research Promotion Scheme (FRPS), Govt. of India, sanctioned to RKS. GBT thanks DST, Govt. of India for financial support. RKS acknowledges, Department of Zoology, Dr. H. S. Gour Central University for providing infrastructural facilities and financial support.
- Ohlsson C, Sjogren K (2014) Effects of the gut microbiota on bone mass Trends Endocrinol Metab 26: 69-74.
- Hamilton-Miller JMT (2004) Probiotics and prebiotics in the elderly. Postgrad Med J 80: 447- 451.
- Ouwehand AC, Salminen S, Isolauri E (2002) Probiotics: an overview of beneficial effects. Antonie van Leeuwenhoek 82: 279-289.
- Panwar H, Rashmi HM, Batish VK, Grover S (2013) Probiotics as potential bio therapeutics in the management of type 2 diabetes-prospects and perspectives. Diabetes Metab Res Rev 29: 103-112.
- Wang Z, Klipfell E, Bennett BJ, Koeth R, Levison BS, (2011) Gut flora metabolism of phosphatidyl choline promotes cardiovascular disease. Nature 472: 57-63.
- Kevin W, Eamonn Q (2013) Probiotics in the management of irritable bowel syndrome and inflammatory bowel disease. Curr Opin Gastroenterol 29: 184-189 .
- National-Osteoporosis-Foundation (2012) National Osteoporosis Foundation National.
- Britton RA, Irwin R, Quach D, Schaefer L, McCabe LR., et al. (2014) Probiotic L. reuteri Treatment Prevents Bone Loss in a Menopausal Ovariectomized Mouse Model. J Cell Physiol 229: 1822-1830.
- Chan KM, Anderson M, Lau EM (2003) Exercise interventions: defusing the world's osteoporosis time bomb. Bulletin of the World Health Organization 81: 827- 830.
- Belkaid Y, Hand TW (2014) Role of the Microbiota in Immunity and Inflammation. Cell 157: 121-141.
- Ohlsson C, Engdahl C, Fa°k F, Andersson A, Windahl SH, et al. (2014) Probiotics Protect Mice from Ovariectomy-Induced Cortical Bone Loss. PLoS One 9: e92368.
- Medzhitov R, Janeway C JR (2000) Innate immune recognition: mechanisms and pathways. Immunol Rev 173: 89-97.
- Akira S, Hemmi H (2003) Recognition of pathogen-associated molecular patterns by TLR family. Immunol Lett 85: 85-95.
- Geuking MB, Cahenzli J, Lawson MA, Ng DC, Slack E, et al. (2011) Intestinal bacterial colonization induces mutualistic regulatory T cell responses. Immunity 34: 794-806 .
- AJ Macpherson, T Uhr (2004) Induction of protective IgA by intestinal dendritic cells carrying commensal bacteria. Science 303: 1662-1665.
- Vaishnava S, Yamamoto M, Severson KM, Ruhn KA, Yu X, et al. (2011) The antibacterial lectin RegIIIgamma promotes the spatial segregation of microbiota and host in the intestine. Science 334: 255-258.
- Cash HL, Whitham CV, Behrendt CL, Hooper LV (2006) Symbiotic bacteria direct expression of an intestinal bactericidal lectin. Science 313: 1126-1130.
- Van Kaer L, Parekh VV, Wu L (2011) Invariant natural killer T cells: bridging innate and adaptive immunity. Cell Tissue Res 343: 43-55.
- Segawa S, Nakakita Y, Takata Y, Wakita Y, Kaneko T, et al. (2008) Effect of oral administration of heat-killed Lactobacillus brevis SBC8803 on total and ovalbumin-specific immunoglobulin E production through the improvement of Th1/Th2 balance. Int J Food Microbiol 121: 1-10.
- Kearns AE, Khosla S, Kostenuik PJ (2008) Receptor activator of nuclear factor kappaB ligand and osteoprotegerin regulation of bone remodeling in health and disease. Endocr Rev 29: 155-192.
- Lorenzo J, Horowitz M, Choi Y (2008) Osteoimmunology: interactions of the bone and immune system. Endocr Rev 29: 403-440.
- Mundy GR (2007) Osteoporosis and inflammation. Nutr Rev 65: S147-S151 .
- Kong YY, Feige U, Sarosi I, Bolon B, Tafuri A, et al. (1999) Activated T cells regulate bone loss and joint destruction in adjuvant arthritis through osteoprotegerin ligand. Nature 402: 304-309.
- Martin-Millan M, Almeida M, Ambrogini E, Han L, Zhao H, et al. (2010) The estrogen receptor-alpha in osteoclasts mediates the protective effects of estrogens on cancellous but not cortical bone. Mol Endocrinol 24: 323-334.
- McCabe LR, Irwin R, Schaefer L, Britton RA (2013) Probiotic use decreases intestinal inflammation and increases bone density in healthy male but not female mice. J Cell Physiol 228: 1793-1798.
- Tomofuji T, Ekuni D, Azuma T, Irie K, Endo Y, et al. (2012) Supplementation of broccoli or Bifidobacterium longum-fermented broccoli suppresses serum lipid peroxidation and osteoclast differentiation on alveolar bone surface in rats fed a high-cholesterol diet. Nutrition Research 32: 301-307.
- Chiang SS, Pan TM (2011) Anti-osteoporotic effects of Lactobacillus-fermented soy skim milk on bone mineral density and the microstructure of femoral bone in ovariectomized mice. J Agric Food Chem. 59: 7734-7742.
- Narva M, Collin M, Lamberg-Allardt C, Kärkkäinen M, Poussa T, et al. (2004) Effects of long-term intervention with Lactobacillus helveticus-fermented milk on bone mineral density and bone mineral content in growing rats. Ann Nutr Metab. 48: 228- 234.
- Ghanem KZ, Badawy IH, Abdel-Salam AM (2004) Influence of yoghurt and probiotic yoghurt on the absorption of calcium, magnesium, iron, and bone mineralization in rats. Milchwissenschaft 59: 472-475.
- Nakamura T, Imai Y, Matsumoto T, Sato S, Takeuchi K, et al. (2007) Estrogen prevents bone loss via estrogen receptor alpha and induction of Fas ligand in osteoclasts. Cell 130: 811- 823 .
- Crittenden RG, Martinez NR, Playne MJ (2003) Synthesis and utilisation of folate by yoghurt starter cultures and probiotic bacteria. Int J Food Microbiol 80: 217-222.
- Weber P (1999) The role of vitamins in the prevention of osteoporosis-a brief status report. Int J Vitam Nutr Res 69: 194-197.
- Villa ML, Marcus R, Ramirez Delay R, Kelsey JL (1995) Factors contributing to skeletal health of postmenopausal Mexican-American women. J Bone Miner Res 10: 1233-1242 .
- Kwon HK, Lee CG, So JS, Chae CS, Hwang JS, et al. (2010) Generation of regulatory dendritic cells and CD4+Foxp3+ T cells by probiotics administration suppresses immune disorders. Proc Natl Acad Sci USA 107: 2159-2164.
- Ohlsson C, Engdahl C, Fak F, Andersson A, Windahl SH, et al. (2014) Probiotics Protect Mice from Ovariectomy-Induced Cortical Bone Loss. PLoS One 9: e92368 .
- Ochi S, Shinohara M, Sato K, Gober HJ, Koga T, et al. (2007) Pathological role of osteoclast costimulation in arthritis-induced bone loss. Proc Natl Acad Sci U S A 104: 11394-11399.
- Simonet WS, Lacey DL, Dunstan CR, Kelley M, Chang MS, et al. (1997) Osteoprotegerin: a novel secreted protein involved in the regulation of bone density. Cell 89: 309-319.
- Sato K, Takayanagi H (2006) Osteoclasts, rheumatoid arthritis, and osteoimmunology. Curr Opin Rheumatol 18: 419-426.
- Feldmann M (2002) Development of anti-TNF therapy for rheumatoid arthritis. Nat Rev Immunol 2: 364-371.
- Li P, Schwarz EM, O'Keefe RJ, Ma L, Looney RJ, et al. (2004) Systemic tumor necrosis factor alpha mediates an increase in peripheral CD11b high osteoclast precursors in tumor necrosis factor alpha-transgenic mice. Arthritis Rheum 50: 265-276.
- Kwon HK, Lee CG, So JS, Chae CS, Hwang JS, et al. (2010) Generation of regulatory dendritic cells and CD4+Foxp3+ T cells by probiotics administration suppresses immune disorders. Proc Natl Acad Sci USA 107: 2159-2164.
- Bouladoux N, Hall JA, Grainger JR, dos Santos LM, Kann MG, et al (2012). Regulatory role of suppressive motifs from commensal DNA. Mucosal Immunol 5: 623-634.
- Marie JC, Letterio JJ, Gavin M, Rudensky AY (2005) TGF-beta1 maintains suppressor function and Foxp3 expression in CD4+CD25+ regulatory T cells. J Exp Med 201: 1061 1067.
- Luo CY, Wang L, Sun C, Li DJ (2011) Estrogen enhances the functions of CD4+ CD25+ Foxp3+ regulatory T cells that suppress osteoclast differentiation and bone resorption in vitro. Cell Mol Immunol 8: 50-58.
- Buchwald ZS, Kiesel JR, Yang C, DiPaolo R, Novack DV, et al. (2013) Osteoclast induced Foxp3+ CD8 T-cells limit bone loss in mice. Bone 2013; 56: 163-173.
- Hancock RD, Viola R (2001) The use of micro-organisms for L-ascorbic acid production: current status and future perspectives. Appl Microbiol Biotechnol 5: 567-576.
- Villa ML, Marcus R, Delay RR, Kelsey JL (1995) Factors contributing to skeletal health of postmenopausal Mexican- American women. J Bone Miner Res 10: 1233-1242.
- Weber P (1999) The role of vitamins in the prevention of Osteoporosis-a brief status report. Int J Vitam Nutr Res 69: 194-197.
- Campbell JM, Fahey Jr GC, Wolf BW (1997) Selected indigestible oligosaccharides affect large bowel mass, cecal and fecal short-chain fatty acids, pH and microflora in rats. J Nutr 127: 130-136.
- Li JY (2014) Gut microbiota plays a pivotal role in the bone loss induced by sex steroid deficiency. J Bone Miner Res 29: 1029.
- Ritchlin CT, Haas-Smith SA, Li P, Hicks DG, Schwarz EM (2003) Mechanisms of TNFalpha- and RANKL-mediated osteoclastogenesis and bone resorption in psoriatic arthritis. J Clin Invest 111: 821-831.
- Whelan K, Quigley EM (2013) Probiotics in the management of irritable bowel syndrome and inflammatory bowel disease. Curr Opin Gastroenterol 29:184-189.
- Yan F, Polk DB (2011) Probiotics and immune health. Curr Opin Gastroenterol 27: 496-501.
- Rodrigues FC, Castro, Rodrigues, Fernandes SA, Fontes EAF, et al. (2012) Yacon flour and Bifidobacterium longum modulate bone health in rats. Journal of Medicinal Food 15: 664-670.
- Mutuş R, Kocabagli N, Alp M, Acar N, Eren M, et al. (2006) The effect of dietary probiotic supplementation on tibial bone characteristics and strength in broilers. Poult Sci 85: 1621-1625.
- Kim YG, Lee CK, Nah SS, Mun SH, Yoo B, et al. (2007) Human CD4+CD25+ regulatory T cells inhibit the differentiation of osteoclasts from peripheral blood mononuclear cells. Biochem Biophys Res Commun 357: 1046-1052.
- Narva M, Nevala R, Poussa T, Korpela R (2004) The effect of Lactobacillus helveticus fermented milk on acute changes in calcium metabolism in postmenopausal women. Eur J Nutr 43: 61-68.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
